Passing Down or Inheriting TSC
The pattern of inheritance of TSC in families
A faulty TSC gene can either be passed down (inherited) from a parent or may occur as a new faulty gene just before or after conception. Once a faulty gene is present in an individual’s egg or sperm cells, it can be passed on to future generations. This is referred to as genetic inheritance.
Two factors influence the pattern of inheritance of a faulty TSC gene.
- The TSC genes are located on one of the numbered chromosomes (autosomes), not the sex chromosomes.
- The effect of the faulty TSC gene is ‘dominant’ over the information in the working copy of the gene (see DNA, RNA, genes and chromosomes, Chromosome changes).
The pattern of inheritance in families of the faulty gene causing TSC is therefore described as autosomal dominant inheritance (see Autosomal dominant inheritance).
Only a person with TSC is at risk of passing on TSC to their children. So it is important for family members to know whether they carry a TSC mutation and therefore have TSC. This may be the case even if they show no or few signs of TSC. If the mutation causing TSC in your family has been found, then your blood can be tested to see if you carry the same mutation.
Genetics and TSC
When a parent has TSC
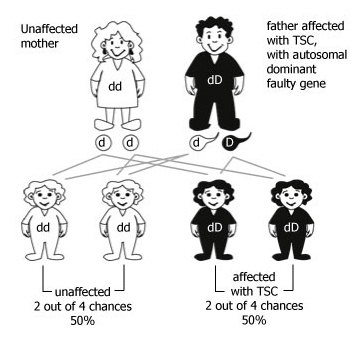
While the picture shows the father as the parent with the faulty TSC gene copy, the same situation would arise if the mother had the faulty TSC gene copy. TSC usually affects men and women equally.
In about 30% of cases, TSC is inherited from an affected parent.
A person diagnosed with TSC has a 50% chance of passing on their TSC gene mutation to any child they have. A child that inherits their gene mutation may be more or less severely affected by TSC than their parent.
A geneticist or a genetic counsellor can be very helpful in helping an individual and their family understand their options and make decisions about having children and prenatal testing.
When one of the parents has TSC due to the faulty TSC gene, there’s a 1 in 2 (50%) chance that they could have a child with TSC. This means that, in each pregnancy:
- If their child inherits the faulty TSC gene, he/she will be affected by TSC.
- If their child inherits the working TSC gene from the affected parent, then the child will not develop TSC and cannot pass on the faulty TSC gene copy to any of their children.
The chance resets in each pregnancy, just like when you are flipping a coin, so having a child with TSC already does not mean that your next child will be unaffected.
If a person with TSC wishes to avoid passing on their TSC gene change to their children, there are several options available. The main options are:
- Preimplantation genetic testing (PGT) is a specialised type of testing offered by IVF (in vitro fertilisation) services. It involves testing for certain genetic conditions in an embryo prior to transferring it to the uterus to establish a pregnancy. Only embryos without the specific genetic condition that was tested for will be transferred.
- Genetic diagnosis through prenatal genetic testing. The two tests most commonly used are Chorionic Villus Sampling (CVS) and Amniocentesis. Each test has its advantages, disadvantages and limitations which must be discussed when deciding if a test is to be done and if so, which test is preferred.
Non-invasive pre-natal testing (NIPT) is a test that uses a sample of the mother’s blood during pregnancy to determine if the developing baby has certain chromosome conditions that can affect health and development. During pregnancy, some of the DNA from the baby (fetal DNA) crosses in to the mother’s bloodstream. This DNA carries the baby’s genetic information. It is this fetal DNA that is tested and analysed during NIPT. Currently in Australia NIPT is available through some specialists to test for chromosome conditions in high risk situations. It does not currently test for individual gene changes, including TSC, and cannot be used to determine if the pregnancy is affected by TSC. This may become available in the future as another option for prenatal genetic diagnosis of TSC.
When neither parent has TSC but they have a child with the condition
In approximately 70% of cases, the person with TSC is the first in the family with the condition. In these people, the condition resulted from a change that occurred in one copy of the TSC1 or TSC2 genes during formation of the egg or sperm, during conception or shortly after. These changes that make one of the TSC gene copies faulty are called ‘spontaneous mutations’. Spontaneous mutations are not caused by any action of the parents but arise by chance, as a new change.
Once a person has TSC s/he may potentially pass on the faulty gene copy to his/her children as described above.
If the TSC gene became faulty shortly after conception, not all of the baby’s cells may contain the gene variation; this individual is said to be ‘mosaic’ for the faulty TSC gene. They may experience milder symptoms because the faulty gene may not be present in all of the organs usually affected in TSC. The faulty gene might not be in all the egg or sperm cells of an individual with mosaic TSC. Their chance of passing on the faulty gene is therefore likely less than 50%. Click here if you want to find out more about mosaicism.
If a child of a parent who is mosaic for TSC inherits the faulty TSC gene copy, they may be more severely affected by TSC than their parent. This is because the child has the faulty gene in all the cells of their body, while their parent only has the faulty gene in some cells. That child also has a 50% risk of passing on the faulty gene copy to his or her future children.
Because of the possibility that an unaffected parent of a child with TSC is mosaic for the faulty TSC gene, the chance of having another child affected by TSC, even if both parents do not carry the faulty TSC gene on testing, is estimated between 1% and 3%. The chance that a spontaneous mutation in the TSC gene would happen again in further pregnancies is low.
TSC does not ‘skip generations’. However sometimes the features of the condition are so subtle that individuals do not realise they have TSC. This is the reason that the international guidelines recommend reviewing the newly diagnosed individual’s nearest three generations (siblings, parents, and either children or grandparents). An assessment by a skin specialist (dermatologist), eye doctor (ophthalmologist) and genetics doctor (clinical geneticist) may be useful in either confirming or ruling out that someone is affected by TSC.
Last updated: 29 April 2025
Reviewed by: Dr Clara Chung, Clinical Geneticist, Sydney Children’s Hospital
Updated October 2022 following review by Dr Clara Chung, Clinical Geneticist, Sydney Children’s Hospital, Dr Fiona McKenzie, Clinical Geneticist, Genetic Services of WA, Dr David Mowat, Clinical Geneticist, Sydney Children’s Hospital
- Peron A, Au KS, Northrup H. Genetics, genomics, and genotype-phenotype correlations of TSC: Insights for clinical practice. Am J Med Genet C Semin Med Genet 2018; 178: 281–290.
- Northrup H, Koenig MK, Pearson DA, et al. Tuberous Sclerosis Complex. 1999 Jul 13 [Updated 2021 Dec 9]. In: Adam MP, Mirzaa GM, Pagon RA, et al., editors. GeneReviews® [Internet]. Seattle (WA): University of Washington, Seattle; 1993-2022. Available from: https://www.ncbi.nlm.nih.gov/books/NBK1220/
- Giannikou K, Lasseter KD, Grevelink JM, Tyburczy ME, Dies KA et al. Low-level mosaicism in tuberous sclerosis complex: prevalence, clinical features, and risk of disease transmission. Genet Med 2019; 21: 2639–2643.
- TSC Alliance, How is TSC diagnosed?, viewed 20th September 2022, https://www.tscalliance.org/about-tsc/how-is-tsc-diagnosed/
- Centre for Genetics Education, Preimplantation genetic diagnosis, viewed 20th September 2022, https://www.genetics.edu.au/SitePages/Preimplantation-genetic-diagnosis.aspx
- Centre for Genetics Education, Diagnostic tests during pregnancy, viewed 20th September 2022, https://www.genetics.edu.au/SitePages/Diagnostic-tests-during-pregnancy.aspx
Parts of this information have been adapted with permission from copyrighted content developed by the TSC Alliance (tscalliance.org).
There is a large amount of helpful information on the website of the Centre for Genetics Education.
